Navigating the waters of health insurance coverage can often be as daunting as dealing with a knee injury itself. For those covered by Medicare, the question of whether or not a knee brace is included in the plan is a common one. As we age, the knees, pivotal to our mobility, are prone to a myriad of issues, from arthritis to post-operative care. This is where the right medical and financial support becomes essential. In this comprehensive guide, we delve into the intricacies of Medicare coverage for knee braces, offering you the knowledge to understand your eligibility, the benefits you’re entitled to, and how to claim them with ease. Whether recovering from surgery or managing chronic pain, understanding your Medicare benefits for knee braces can significantly reduce your physical and financial discomfort.
Understanding Medicare’s Durable Medical Equipment Coverage
Navigating the complex terrain of healthcare coverage is critical for those who rely on medical aids for daily living and recovery. Medicare, a federal health insurance program, offers a lifeline for many, particularly in covering Durable Medical Equipment (DME) — a term that encompasses a wide range of medical aids, including knee braces, which are indispensable for individuals dealing with knee injuries or conditions.
When you’re faced with a knee condition that impedes your mobility or causes chronic pain, the support of a knee brace can be a game changer. Such medical devices are engineered to offer stability, reduce pain, and facilitate the healing process. Medicare’s coverage of these devices ensures that beneficiaries can access the essential support they need without the full cost burden.
What Qualifies as Durable Medical Equipment?
Durable Medical Equipment refers to medical items that are prescribed by a doctor for a patient’s use at home and can withstand repeated use. They are essential aids for various health conditions and recovery processes. Under Medicare Part B, DME coverage encompasses a wide range of equipment, with knee braces being one of the many items provided for those who require them for medical reasons.
To qualify for a Medicare-covered knee brace, your doctor must first confirm that it is medically necessary. This typically means the brace must serve a therapeutic function, aiding in recovering an injury or managing a medical condition such as osteoarthritis.
The Specifics of Knee Brace Coverage
Let’s delve deeper into the coverage specifics for knee braces. Medicare recognizes the variability in the medical needs and conditions of each patient and, therefore, the need for different types of braces. As a rule of thumb, the brace should be a medical-grade device, not just an off-the-shelf product that you can pick up at any store. Here’s a little more detail on the types of braces that are typically covered:
- Basic Knee Supports: These are often used for minor knee pain and injuries. They can help provide a level of compression and support that may alleviate pain and encourage stability in the knee joint.
- Advanced Orthotic Supports: For more severe conditions, such as post-operative recovery or significant ligamentous injuries, an advanced orthotic may be necessary. These devices are usually custom-fitted and designed to limit certain movements that could delay healing or cause further injury.
Medicare will cover the cost of these knee braces if they’re deemed medically necessary—meaning they’re needed to treat or correct a medical condition or injury. It’s not enough for a brace to simply provide comfort; it must have a therapeutic benefit.
Eligibility Requirements for Knee Brace Coverage
The eligibility for a knee brace under Medicare’s DME coverage hinges on the brace being medically necessary for a diagnosed condition and prescribed by a Medicare-enrolled provider who can substantiate its necessity with detailed documentation. Understanding and complying with these requirements can significantly streamline the process and help ensure that you receive the support you need.
Qualifying Conditions
Medicare’s eligibility criteria for covering a knee brace under DME are quite specific. The program typically provides coverage when the brace is deemed medically necessary due to conditions that inhibit mobility or cause significant pain. These conditions can range from degenerative diseases like osteoarthritis to more acute issues such as injuries from falls or sports activities. Post-operative recovery is another scenario where knee braces are commonly prescribed and covered.
The key factor is that the use of the knee brace must relate directly to a diagnosed medical condition, and it must be integral to managing or treating that condition. It is not enough for a brace to simply provide comfort; there must be a therapeutic benefit that aids in the patient’s rehabilitation or improves their ability to perform daily activities.
Doctor’s Prescription and Documentation
Obtaining a prescription is the first step in the process. But it’s not just any prescription — Medicare requires detailed documentation from the healthcare provider. This means that your doctor or specialist must provide a written order that clearly states:
- The medical reason for the knee brace (e.g., diagnosis of a knee injury or condition).
- The expected benefits of using the brace.
- The length of time you will need to use the brace.
The documentation must be thorough enough to convince Medicare that the knee brace is necessary for your treatment plan. Your healthcare provider should also specify the type of knee brace required — whether it’s a basic support brace, a post-surgical brace with hinges, or a custom-fitted orthotic — as different types of braces may have different eligibility requirements.
Read More: Knee Braces after Arthritis Surgery: What You Need to Know?
How to Obtain a Medicare-Covered Knee Brace?
Securing a knee brace through Medicare requires several steps to ensure that all the necessary conditions and procedures are followed for coverage. Here’s a guide to navigating the process:
Finding the Right Supplier
The first step is to find a supplier that is enrolled in the Medicare program and has been approved to provide Durable Medical Equipment (DME). Not all suppliers accept Medicare, so this is a crucial step.
- Medicare’s Supplier Directory: You can use the supplier directory on Medicare’s official website to find approved suppliers in your area. This tool allows you to search by zip code and the type of equipment you need.
- Check for Competitive Bidding: Medicare uses a competitive bidding program for DME in some areas. This means that you must obtain your knee brace from a supplier that has been awarded a Medicare contract under this program in your area.
- Verify Supplier Authorization: Even if a supplier is listed in the directory, it’s a good idea to call and confirm that they are still participating in Medicare and accept the terms of the program.
The Approval and Claims Process
After locating an approved supplier, the next steps involve getting the brace and submitting a claim.
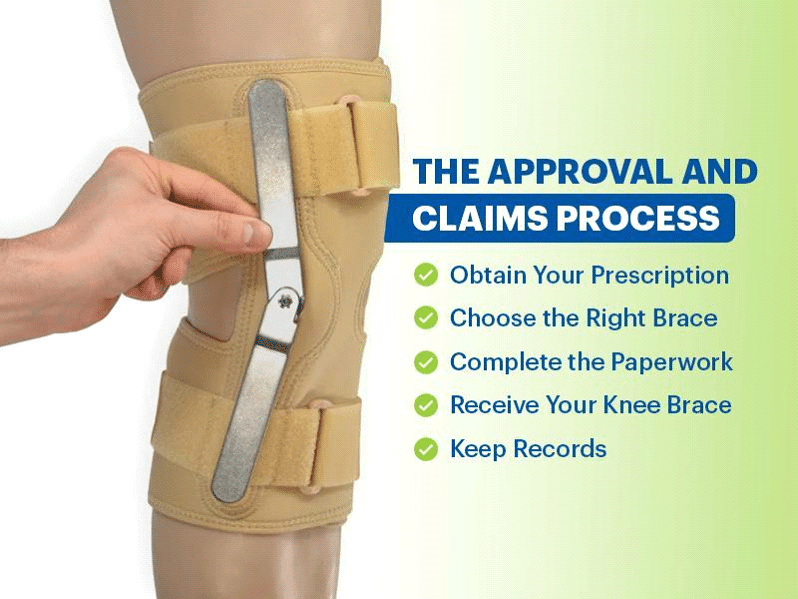
- Obtain Your Prescription: You will need a detailed prescription from your healthcare provider. Make sure it includes all the necessary information as per Medicare’s requirements.
- Choose the Right Brace: With the help of the supplier, select a knee brace that fits the prescription specifications and is covered by Medicare.
- Complete the Paperwork: The supplier should help you with all the necessary paperwork, which typically includes the prescription, a Medicare claim form, and any additional documentation from your doctor.
- Receive Your Knee Brace: Once the paperwork is processed and approved, you can receive your knee brace. Some suppliers will bill Medicare directly, while others may require you to pay upfront and seek reimbursement.
- Keep Records: Maintain a copy of all forms, prescriptions, and communication in case of any future disputes or inquiries from Medicare.
Maximizing Your Benefits
Navigating the details of your Medicare coverage is essential to maximizing the benefits you are entitled to, particularly when it comes to obtaining a knee brace. Here’s how to understand your plan and handle costs and reimbursements:
Understanding Your Plan

It’s crucial to know the intricacies of your specific Medicare plan, as coverage can vary. Here are some tips:
- Review Your Summary of Benefits: Your Medicare plan’s summary of benefits outlines what’s covered and to what extent. Review this document closely to understand the specifics of DME coverage.
- Know the Difference Between Parts A, B, C, and D: Medicare Part B typically covers DME, but Medicare Advantage Plans (Part C) may have different rules and coverage limits.
- Supplemental Insurance Consideration: If you have a Medigap or other supplemental insurance policy, check to see if it offers additional coverage or helps with costs that Medicare doesn’t fully cover.
Costs and Reimbursements
Understanding the financial aspects is equally important. Here’s what you should know:
- Out-of-Pocket Costs: Even with Medicare, you may be responsible for a portion of the costs, such as deductibles and co-insurance. Ensure you understand these potential expenses upfront.
- Reimbursement Process: If you pay out-of-pocket, you’ll need to submit a claim form to Medicare or your supplemental insurer for reimbursement. Keep detailed receipts and records of all transactions related to the knee brace.
- Cap on Expenses: Some Medicare plans have out-of-pocket maximums, after which all covered services are paid at 100%. Know where this cap is set for your plan.
Conclusion
Understanding the details of your Medicare coverage is key when it comes to accessing necessary medical equipment like knee braces. These braces can play a significant role in your recovery process, aiding in mobility and pain relief, which can dramatically improve your quality of life. Stay informed, ask questions, and work closely with your healthcare provider and DME suppliers to ensure you are getting the support you need while maximizing your Medicare benefits.
Tags
- Medicare Coverage
- Knee Braces
- Durable Medical Equipment
- Health Insurance
- Orthopaedic Support
Keyphrase
Medicare coverage for knee braces
Keyphrase Synonym
- Medicare eligibility for orthopaedic braces
- knee braces covered by Medicare
- Does Medicare cover knee braces
- how to get knee braces covered by insurance
- how often will Medicare pay for knee braces
- are knee braces covered by Medicare
- what knee braces are covered by Medicare